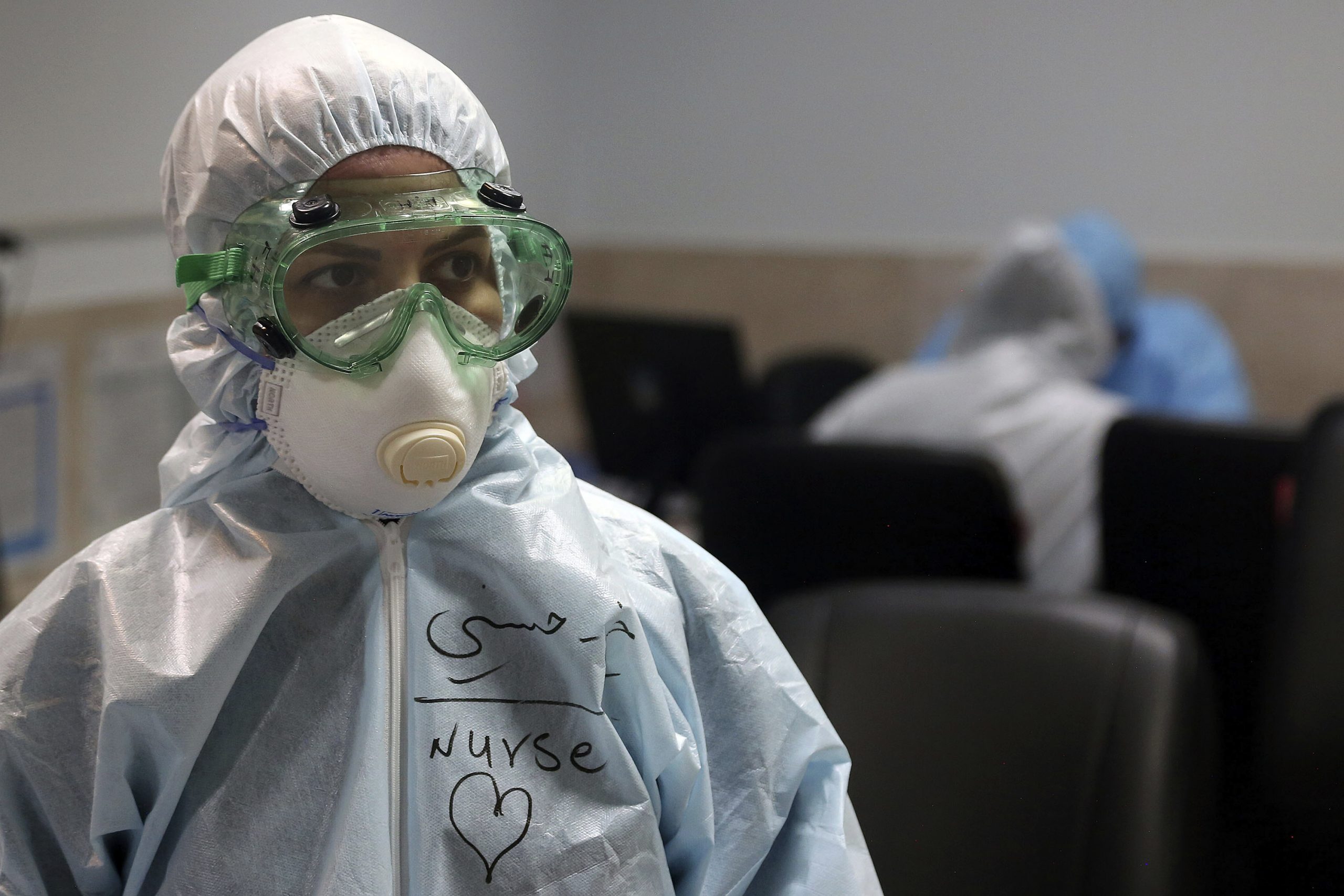
Narjes Khanalizadeh was a 25-year-old nurse in Gilan, a province along the Caspian Sea in northern Iran. In late February, after working with coronavirus patients at a hospital in the city of Lahijan, she fell sick. Within a few days, she was dead.
A week later, results from a coronavirus test that had been administered before her death came back positive, sparking anger and fear among the country’s nurses. Khanalizadeh, who had been working without adequate protective gear, is one of more than a dozen nurses who have died from the coronavirus since February, despite desperate warnings from nurses about shortages of personal protective equipment at hospitals, including at Khanalizadeh’s.
Upwards of 100 Iranian health workers have died from the coronavirus, prompting Iranian Supreme Leader Ayatollah Ali Khamenei to announce in March that doctors and nurses who die from the infection will be recognized as “martyrs,” an honorific usually used for soldiers who sacrifice themselves in battle and that authorizes the families of the deceased to receive certain benefits, such as subsidized housing and education. But Iran’s official response to the crisis has been slow and inefficient, and U.S. sanctions are making things worse. In 2018, U.S. President Donald Trump pulled out of the Iran nuclear deal and reimposed harsh economic sanctions on the country, hampering access to desperately needed medical supplies and equipment.
Now, Iran’s nurses—the majority of whom are women—are among those bearing the worst of the brunt of U.S. sanctions. Official death counts from the Iranian government aren’t broken out by profession and are widely believed to understate coronavirus fatalities. A group of doctors in Iran that has been tracking the deaths of health care workers puts the number of nurses who have died at at least 15 between late February and mid April, but even that almost certainly underestimates the toll as health workers have reportedly been instructed by government officials not to reveal information about shortages, infections, or deaths. Dozens more nurses have been infected, in part as a result of restrictions imposed by the Trump administration.
U.S. sanctions on medical supplies
While food and medicine are exempt from U.S. sanctions, many medical supplies and certain types of equipment are not. To sell some protective items to Iran, including full face mask respirators and some decontamination systems used to sterilize them, companies need a special license from the U.S. Treasury Department (see here for a list of items requiring special authorization). In March, the Washington Post reported that the Trump administration has reduced the number of licenses granted to companies that export medical supplies to Iran.
Even when a license isn’t required to ship humanitarian items, some companies and banks avoid doing business with Iran altogether for fear of being penalized. The country also has far fewer financial resources available to purchase necessary supplies due to sanctions. “This year, Iran is running its largest ever fiscal deficit—50 percent of its budget,” said Hadi Kahalzadeh, a former economist for Iran’s Social Security Organization. “Iran’s health sector, especially hospitals and pharmacies, don’t have enough liquidity to purchase essential supplies. And the Iranian government doesn’t have the financial means to fill the gap.”
Alan Veisi, a biomechanics engineer at Baran MicroTech, a company in Iran that produces some medical equipment that the country isn’t able to import due to sanctions, said even one of Tehran’s most prominent hospitals, Imam Khomeini, has shortages of N95 masks, gloves, and protective gear. “They need 500 to 1000 masks every day,” he said. “But get only 300.” Other hospitals are experiencing similar shortages.
For Iran’s nurses, the risks of contracting the coronavirus are compounded by low wages, poor working conditions, and severe overwork. It begins with the fact that there are far too few of them. According to World Bank data from 2015, Iran has 1.9 nurses per 1,000 people, compared with 2.3 in China, 5.9 in Italy (in 2017), and 8.6 in the United States. Iran’s nurses are under intense psychological pressure, working long hours and even sleeping at hospitals. Some haven’t seen their children or families for days or weeks.
The toll hasn’t been merely psychological. Testing in Iran has so far been restricted only to severe cases, so the dozens of officially reported infections among nurses are likely a vast undercount. Meanwhile, the number of Iranian nurses who have died from the coronavirus is roughly on par with the number of nurses who have died in Italy, even though the official overall death toll there is more than four times higher, suggesting that Iranian nurses are disproportionately at risk. Many experts and human rights groups also believe the Iranian government is underreporting coronavirus deaths to dispel criticism of its response.
Where official mismanagement and harsh U.S sanctions are failing Iranian nurses and health care workers, nonprofit organizations are partially stepping into the void. Some of the need for protective equipment is being filled by humanitarian groups that already have licenses from the U.S. government to operate in Iran. One of these organizations, Relief International, has been importing N95 masks and Tyvek 400 protective coveralls. UNICEF Iran has also been importing two types of high-filtered respiratory surgical masks, N95 masks, and surgical gowns for Iranian health personnel. But even these organizations have had to overcome supplier reluctance to ship to Iran, and the need for protective equipment far surpasses what they are able to provide.
Reliance on foreign equipment and raw materials
Domestic producers have picked up some of the slack, but many medical supplies produced in Iran still rely on foreign equipment and raw materials imported from abroad—at prices far higher than what they would get if they could buy from countries directly. “Iranian importers have to pay around 30 to 50 percent more for goods through third countries,” said Bijan Khajehpour, a managing partner at Eurasian Nexus Partners. “This means that for a total annual import figure of $50 billion, Iran will end up paying about $15 billion more than the value of the goods.”
There is bipartisan precedent in the United States for sanctions relief for Iran in times of crisis. After an earthquake devastated the country in 2003, the usually hawkish George W. Bush administration eased sanctions for three months to expedite aid and assistance. The Obama administration took similar measures after another earthquake hit Iran in 2012, easing sanctions for 45 days to facilitate humanitarian aid.
But despite both domestic and international calls for Trump to follow suit, the current administration is showing no signs of giving Iran any relief during the pandemic, other than vaguely worded offers to “assist the Iranian people in their response efforts.” Tehran rejected the overture as “insincere” and politically motivated. Last week, the State Department called the Iranian government’s requests for broader sanctions relief a “scam,” and the Trump administration has said it will block Iran’s request for $5 billion in emergency assistance from the International Monetary Fund to deal with the outbreak.
In March, Mohammad Sharifi Moghaddam, the head of a leading nurses’ union in Iran, told a local news organization that the death toll for nurses in Iran during the coronavirus pandemic has been “unnatural” compared with other countries that have been hit hard by the virus, blaming government mismanagement, staff shortages, and lack of protective equipment. While there is little question that the Iranian government’s response to the coronavirus has been a failure, U.S. sanctions have made the situation worse by disrupting other avenues for humanitarian aid—and the likely result is many more Iranian nurses and health care workers being made into martyrs.


 Negar Mortazavi
Negar Mortazavi